The city is seeing an “uptick” in COVID-19, flu and respiratory syncytial virus cases, Mayor Eric Adams said this week, and health officials are warning that the so-called “triple threat” of the three illnesses could worsen in the coming months.
Here’s what you need to know about the viruses, from how to protect yourself from them to how many infections the city is seeing.
What is respiratory syncytial virus?
Respiratory syncytial virus, or RSV, is a respiratory virus that usually causes cold-like symptoms, including a runny nose, poor appetite, coughing, sneezing, fever and wheezing, the Centers for Disease Control and Prevention says.
The virus can spread via coughs, sneezes, surfaces and direct contact, according to the CDC. Most people who get infected experience mild symptoms and recover within a week or two, but the virus “can be serious, especially for infants and older adults,” the CDC says.
“Each year in the United States, an estimated 58,000 children younger than 5 years old are hospitalized due to RSV infection,” the CDC says on its website.
Premature infants, children who have weakened immune systems and children under the age of 2 who have chronic lung disease are among those most susceptible to “severe illness,” the CDC notes.
Why has RSV been in the news recently?
While RSV usually circulates in the late fall, winter and spring, the U.S. has seen an early surge in pediatric RSV cases this year that has put a strain on some hospitals.
The New York City Department of Health and Mental Hygiene logged around 400 positive RSV test results the week of Sept. 17, according to the department’s most recent influenza surveillance report.
By the week of Oct. 15, that number had jumped to around 1,600 — up by 60% from the same week last year, when the department recorded close to 1,000 RSV cases.
Nationwide, 7,993 RSV test results came back positive the week of Oct. 15, up from 3,034 the week of Sept. 17 and nearly double the 4,005 positive results that came back the week of Oct. 16 last year, CDC data shows.
Dr. Edith Bracho-Sanchez, a pediatrician at NewYork-Presbyterian/Columbia University Irving Medical Center, said in a hospital Q&A video that the facility is “definitely seeing an uptick in respiratory illnesses, including but not limited to RSV.”
“Unfortunately, they came earlier than we’re used to, and they came in higher numbers this season,” Bracho-Sanchez said.
In an interview with NY1, Dr. Jessica Justman, an infectious disease specialist and epidemiologist who serves as associate professor of medicine in epidemiology at Columbia Mailman School of Public Health, said she wasn’t surprised by the increase.
“We’ve now had a couple of winters of people being more careful than usual, masking and staying in, and so people have had less exposure to flu and respiratory syncytial virus for a couple of years,” Justman said. “And so I think that our immune systems are, a little bit, in a lower state of response for these pathogens.”
What do health officials mean by a “triple threat”?
Health officials have been referring to the combination of RSV, COVID-19 and flu as a “triple threat” because they are all circulating simultaneously — and could all fuel a spike in respiratory illnesses in the coming months.
In an interview with Spectrum News, the White House’s COVID-19 response coordinator, Dr. Ashish Jha, said he was worried about the confluence of the three viruses.
“It is concerning to see three respiratory viruses, all of which are very contagious, all of which are rising at the same time,” Jha said.
Justman noted that the city “[hasn’t] really had a winter yet where all three infections are circulating at high levels.”
“I think… in talking about the ‘triple threat,’ I’d emphasize the word ‘threat,’” she added. “It’s something to potentially anticipate and be prepared for, but it doesn’t mean that it’s already here.”
Where do COVID-19 and flu stand in New York City currently?
As of Thursday, New York City’s seven-day infection rate stood at 9.0%, down from 9.3% on Wednesday. COVID-19-related deaths were holding steady, with hospitalizations on the decline, the health department said.
“Influenza activity” in the city, meanwhile, was still “low” as of Oct. 15, according to the department’s influenza surveillance report.
“Approximately 1% of all specimens submitted for influenza testing were positive for influenza; 390 specimens were positive for influenza A and 25 specimens were positive for influenza B,” the report said.
The city did see two flu outbreaks at long-term care facilities the week of Oct. 15, but did not see any “influenza-associated pediatric deaths,” the report added.
Asked about the “triple threat” at a news conference on Wednesday, the mayor said the city was “seeing an uptick” in flu, COVID-19 and RSV cases, but added that it wasn’t a concern for hospitals.
“We believe our health care infrastructure system, we’re in a good place. We have it under control,” Adams said. “And so there’s no real alarms that we’re seeing now, but we want to continue to encourage boosters, vaccines. That’s the key.”
How can you tell which virus you or your child has?
Distinguishing between the viruses’ symptoms can be difficult, health care providers say.
“We have this situation that we haven’t really encountered before, and they all kind of overlap a bit in their symptoms and presentation, so it kind of introduces a level of confusion,” Dr. Denis Nash, a distinguished professor of epidemiology at the CUNY School of Public Health, said in an interview with NY1.
“I think if you have any symptoms, you have to assume that it’s one of these three things, none of which are good for anyone else, and to sequester, isolate,” Nash added.
In her video Q&A, Bracho-Sanchez, acknowledged that it “is so hard to tell the difference between RSV, COVID and flu, even for us as physicians.”
“As a parent, know that [with] most illnesses, whether respiratory illnesses or in cold and flu season, most kids are totally fine at home,” she said. “But always, always be on the lookout for difficulty breathing, a fever that lasts longer than three days, or a fever in a kid who’s younger than two months.”
Justman, meanwhile, noted that it is “possible to have, in theory… an infection with all three viruses at the same time.”
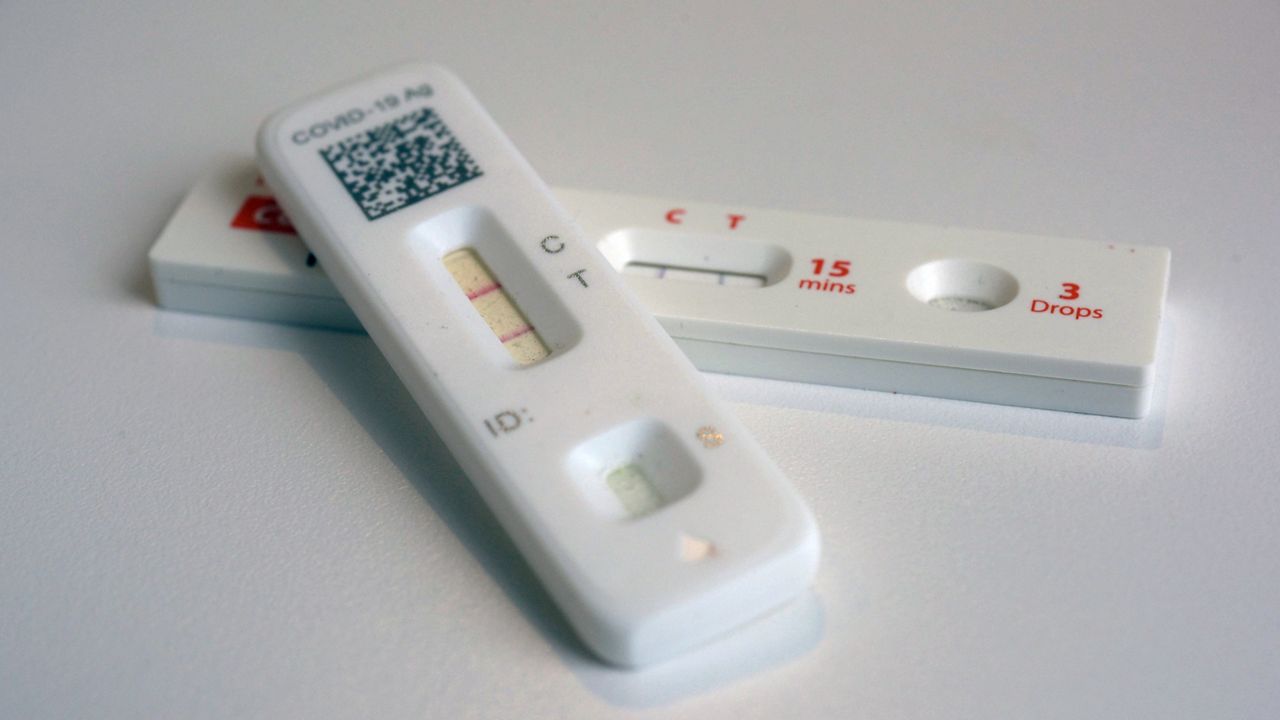
“We have better access to COVID rapid tests, so that will be helpful,” she said, but added that New Yorkers would have to visit a hospital or health care provider’s office to get tested for other “respiratory pathogens.”
What can New Yorkers do to prevent illness?
While there is no vaccine to prevent RSV — only preventive treatments given to high-risk children under the age of 2 — New Yorkers can heed the advice they have heard repeatedly throughout the pandemic to avoid infections, Justman said.
New Yorkers should wash their hands frequently, avoid touching their faces and use hand sanitizer, as the virus “will live on surfaces,” she said. And as with COVID-19, masks will help prevent flu and RSV infections.
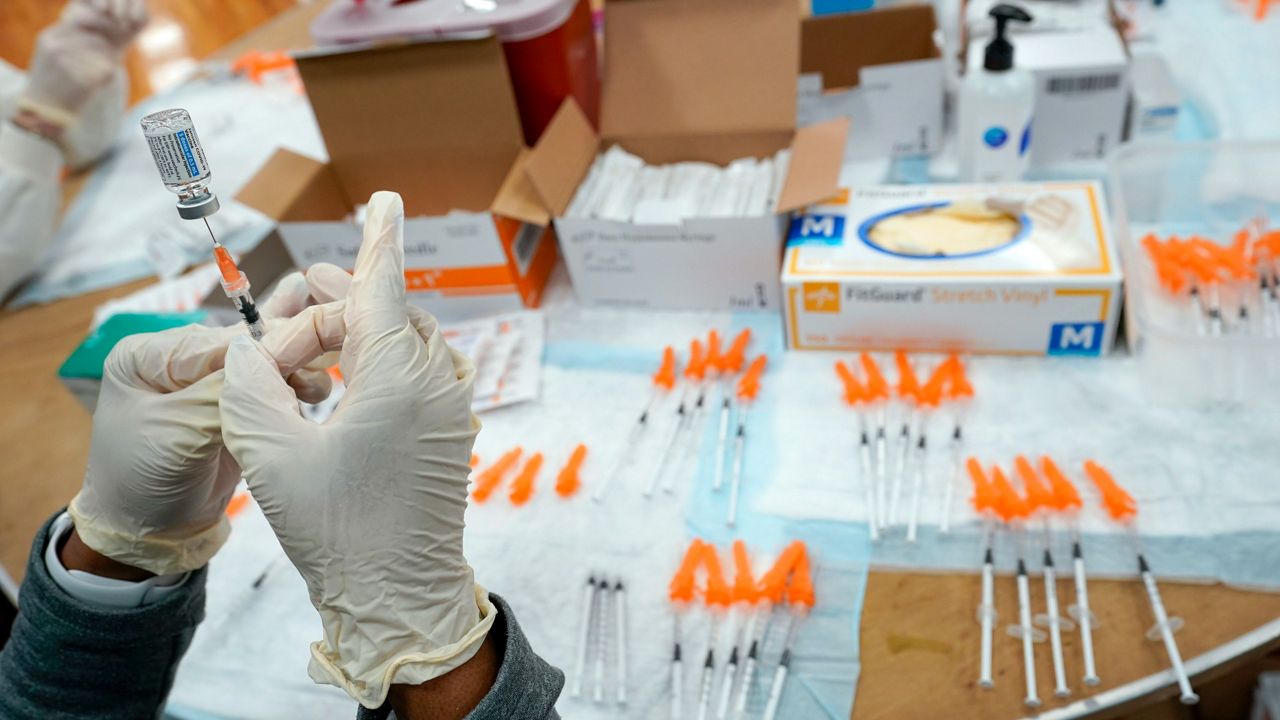
“So if you are at all willing to wear masks still, it will help protect you against all three viruses,” Justman said. New Yorkers should also make sure to get their bivalent COVID-19 booster shots and flu shots, she added.
As of two weeks ago, the city had only administered around 363,000 bivalent booster shots, health officials said. Low bivalent booster rates could push hospitalizations upward, Justman noted.
“The major potential issue would be overwhelming our hospital systems with people who have severe respiratory tract infections,” like pneumonia, she said.
“At the early stages of the COVID-19 pandemic, we heard about the importance of ‘flattening the curve’ in order to preserve hospital bed capacity,” she added. “This would be the same issue, but instead of COVID-19 as the only ‘driver,’ it would potentially be driven by all three respiratory viruses.”
What will the next few months look like for the city?
Nash on Thursday said it would be difficult to pinpoint a potential “peak” in infections.
“It seems to be increasing now, but we’ve never really had a situation where all three of these pathogens were circulating at once,” he said. “I think the interplay between them, since we don’t know how it could play out, makes it a little hard to predict.”
New York will either see case counts comparable to other parts of the country or deal with a “more severe experience” due to its density, Justman said.
“And things that can spread through respiratory transmission just tend to really do that particularly well in densely populated areas,” she said, adding that international travel into and out of the city could fuel cases.
Like Justman, Bracho-Sanchez emphasized taking basic hygiene precautions. She also advised parents with concerns about RSV or other viruses to reach out to their children’s health care providers.
“It’s really hard to know what’s going to happen the rest of the fall and winter, but I think we’re going to continue to see high levels of RSV circulating in our community,” she said in her Q&A. “We are also going to see flu begin to circulate soon, in even higher levels than we have seen, and we might have a wave of COVID-19 circulating in our community, in addition to [other] viruses that we don’t often test for.”